Croup
Viral croup; Laryngotracheobronchitis; Spasmodic croup; Barking cough; Laryngotracheitis
Croup is an infection of the upper airways that causes breathing difficulty and a "barking" cough. Croup is due to swelling around the vocal cords. It is common in infants and children.
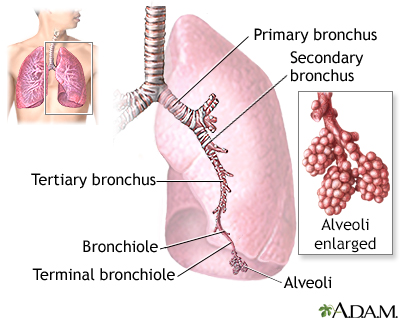
The major features of the lungs include the bronchi, the bronchioles and the alveoli. The alveoli are the microscopic blood vessel-lined sacks in which oxygen and carbon dioxide gas are exchanged.
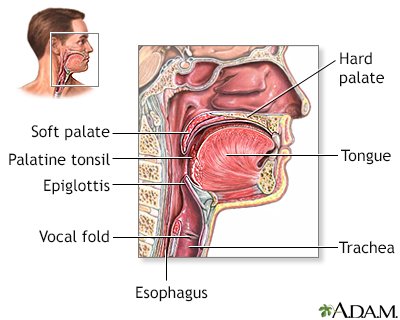
Structures of the throat include the esophagus, trachea, epiglottis and tonsils.
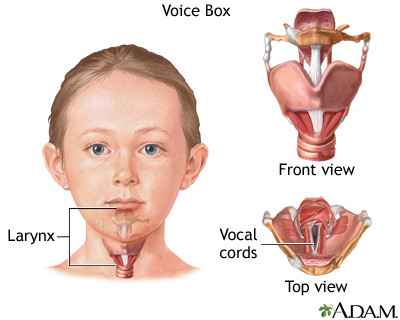
The larynx, or voice box, is located in the neck and performs several important functions in the body. The larynx is involved in swallowing, breathing, and voice production. Sound is produced when the air which passes through the vocal cords causes them to vibrate and create sound waves in the pharynx, nose and mouth. The pitch of sound is determined by the amount of tension on the vocal folds.
Causes
Croup affects children ages 3 months to 5 years. It can occur at any age. Some children are more likely to get croup and may get it several times. It is most common between October and April, but can occur at any time of the year.
Croup is most often caused by viruses such as parainfluenza RSV, measles, adenovirus, and influenza. More severe cases of croup may be caused by bacteria. This condition is called bacterial tracheitis.
Croup-like symptoms may also be caused by:
- Allergies
- Breathing in something that irritates your airway
- Acid reflux
Symptoms
The main symptom of croup is a cough that sounds like a seal barking.
Most children will have mild cold and low grade fever for several days before having barking cough and a hoarse voice. As the cough gets more frequent, the child may have trouble breathing or stridor (a harsh, crowing noise made when breathing in).
Croup is typically much worse at night. It often lasts 5 or 6 nights. The first night or two are most often the worst. Rarely, croup can last for weeks. Talk to your child's health care provider if croup lasts longer than a week or comes back often.
Exams and Tests
Your provider will take a medical history and ask about your child's symptoms. The provider will examine your child's chest to check for:
- Difficulty breathing in and out
- Whistling sound (wheezing)
- Decreased breath sounds
- Chest retractions with breathing
An exam of the throat may reveal a red epiglottis. In a few cases, x-rays or other tests may be needed.
A neck x-ray may reveal a foreign object or narrowing of the trachea.
Treatment
Most cases of croup can be safely managed at home. However, you should call your provider for advice, even in the middle of the night.
Steps you can take at home include:
- Expose your child to cool or moist air, such as in a steamy bathroom or outside in the cool night air. This may offer some breathing relief.
- Set up a cool air vaporizer in the child's bedroom and use it for a few nights.
- Make your child more comfortable by giving acetaminophen. This medicine also lowers a fever so the child will not have to breathe as hard.
- Avoid cough medicines unless you discuss them with your provider first.
Your provider may prescribe medicines, such as:
- Steroid medicines taken by mouth or through an inhaler
- Antibiotic medicine (for some, but not most cases)
Your child may need to be treated in the emergency room or to stay in the hospital if they:
- Have breathing problems that do not go away or get worse
- Become too tired because of breathing problems
- Have bluish skin color
- Are not drinking enough fluids
Medicines and treatments used at the hospital may include:
- Breathing medicines given with a nebulizer machine
- Steroid medicines given through a vein (IV)
- An oxygen tent placed over a crib
- Fluids given through a vein for dehydration
- Antibiotics given through a vein
Rarely, a breathing tube through the nose or mouth will be needed to help your child breathe.
Outlook (Prognosis)
Croup is most often mild, but it can still be dangerous. It most often goes away in 3 to 7 days.
The tissue that covers the trachea (windpipe) is called the epiglottis. If the epiglottis becomes infected, the entire windpipe can swell shut. This is a life-threatening condition.
If an airway blockage is not treated promptly, the child can have severe trouble breathing or breathing may stop completely.
When to Contact a Medical Professional
Most croup can be safely managed at home with telephone support from your provider. Call your provider if your child is not responding to home treatment or is acting more irritable.
Call 911 or the local emergency number right away if:
- Croup symptoms may have been caused by an insect sting or inhaled object.
- Your child has bluish lips or skin color.
- Your child is drooling.
- Your child is having trouble swallowing.
- There is stridor (a noise when breathing in).
- There is a tugging-in of the muscles between the ribs when breathing in.
- Your child is struggling to breathe.
Prevention
Some of the steps to be taken to prevent infection are:
- Wash your hands frequently and avoid close contact with people who have a respiratory infection.
- Timely immunizations. The diphtheria, Haemophilus influenzae (Hib), and measles vaccines protect children from some of the most dangerous forms of croup.
References
Chi DH, Tobey A. Otolarngology. In: Zitelli BJ, McIntire SC, Nowalk AJ, Garrison J, eds. Zitelli and Davis' Atlas of Pediatric Physical Diagnosis. 7th ed. Philadelphia, PA: Elsevier; 2023:chap 24.
Cai Y, Meyer A. Pediatric infectious disease. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 201.
James P, Hanna S. Upper airway obstruction in children. In: Bersten AD, Handy JM, eds. Oh's Intensive Care Manual. 8th ed. Philadelphia, PA: Elsevier; 2019:chap 106.
Rodrigues KK, Roosevelt GE. Acute inflammatory upper airway obstruction (croup, epiglottitis, laryngitis, and bacterial tracheitis). In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 412.
Rose E. Pediatric respiratory emergencies: upper airway obstruction and infections. In: Walls RM, Hockberger RS, Gausche-Hill M, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:chap 167.
Version Info
Last reviewed on: 2/24/2022
Reviewed by: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
