Compartment syndrome
Fracture - compartment syndrome; Surgery - compartment syndrome; Trauma - compartment syndrome; Muscle bruise - compartment syndrome; Fasciotomy - compartment syndrome
Acute compartment syndrome is a serious condition that involves increased pressure in a muscle compartment. It can lead to muscle and nerve damage and problems with blood flow.
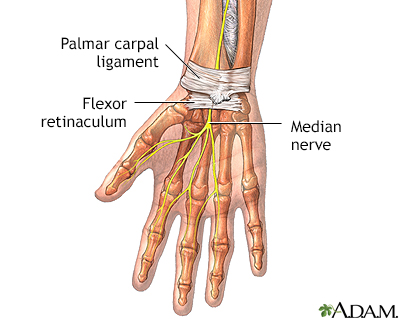
The median nerve travels through a compartment called the carpal tunnel in the wrist. The ligaments that transverse the nerve are not very flexible. If there is any swelling within the wrist compartment excessive pressure can be put on structures such as the blood vessels and the median nerve. Excessive pressure can constrict bloodflow and cause nerve damage. The symptoms from the compression causes pain, loss of sensation, and decreased function in the hand.
Causes
Thick layers of tissue, called fascia, separate groups of muscles in the arms and legs from each other. Inside each layer of fascia is a confined space, called a compartment. The compartment includes the muscle tissue, nerves, and blood vessels. Fascia surrounds these structures, similar to the way in which insulation covers wires.
Fascia do not expand. Any swelling in a compartment will lead to increased pressure in that area. This raised pressure, presses the muscles, blood vessels, and nerves. If this pressure is high enough, blood flow to the compartment will be blocked. This can lead to permanent injury to the muscle and nerves. If the pressure lasts long enough, the muscles may die and the arm or leg will no longer work. Surgery or even amputation may be done to correct the problem.
Acute compartment syndrome may be caused by:
- Trauma, such as a crush injury or surgery
- Broken bone
- Very bruised muscle
- Severe sprain
- A cast or bandage that is too tight
- Loss of blood supply due to the use of a tourniquet or positioning during surgery
Exertional compartment syndrome can be caused by repetitive activities, such as running. The pressure in a compartment only increases during that activity and goes down after the activity is stopped. This condition is usually less limiting and does not lead to loss of function or limb. However, the pain can limit activity and endurance. There is usually no permanent injury to the limb.
Compartment syndrome is most common in the lower leg and forearm. It can also occur in the hand, foot, thigh, buttocks, and upper arm.
Symptoms
Symptoms of compartment syndrome are not easy to detect. With an acute injury, the symptoms can become severe within a few hours.
Symptoms may include:
- Pain that is much higher than expected with the injury
- Severe pain that doesn't go away after taking pain medicine or raising the affected area
- Decreased sensation, numbness, tingling, weakness of the affected area
- Paleness of skin
- Swelling or inability to move the affected part
Exams and Tests
The health care provider will perform a physical exam and ask about the symptoms, focusing on the affected area. To confirm the diagnosis, the provider may need to measure the pressure in the compartment. This is done using a needle placed into the affected body area. The needle is attached to a pressure meter. The test is done during and after an activity that causes pain.
Treatment
The aim of treatment is to prevent permanent damage. For acute compartment syndrome, surgery is needed right away. Delaying surgery can lead to permanent damage. The surgery is called fasciotomy and involves cutting the fascia to relieve pressure.
For chronic compartment syndrome:
- If a cast or bandage is too tight, it should be cut or loosened to relieve the pressure
- Stopping the repetitive activity or exercise, or changing the way it's done
- Raising the affected area above heart level to decrease swelling
Outlook (Prognosis)
With prompt diagnosis and treatment, the outlook is excellent and the muscles and nerves inside the compartment will recover. However, the overall outlook is determined by the injury that led to the syndrome.
If the diagnosis is delayed, permanent nerve injury and loss of muscle function can result. This is more common when the injured person is unconscious or heavily sedated and cannot complain of pain. Permanent nerve injury can occur after less than 12 to 24 hours of compression. Muscle injuries can occur even faster.
Possible Complications
Complications include permanent injury to nerves and muscles that can dramatically impair function. This is called Volkmann ischemic contracture if it occurs in the forearm.
In more severe cases, amputation may be required.
When to Contact a Medical Professional
Contact your provider right away if you have had an injury and have severe swelling or pain that does not improve with pain medicines.
Prevention
There is probably no way to prevent this condition. Early diagnosis and treatment helps prevent many of the complications. At times, fasciotomies are performed earlier to avoid compartment syndrome from occurring in the case of severe trauma.
If you wear a cast, see your provider or go to the emergency room if pain under the cast increases, even after you have taken pain medicines and raised the area.
References
Malekpour F, Modrall JG. Compartment syndrome and its management. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 105.
Stevanovic MV, Sharpe F. Compartment syndrome and Volkmann ischemic contracture. In: Wolfe SW, Pederson WC, Kozin SH, Cohen MS, eds. Green's Operative Hand Surgery. 8h ed. Philadelphia, PA: Elsevier; 2022:chap 51.
Thompson NB. Compartment syndrome and Volkmann contracture In: Azar FM, Beaty JH, eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 74.
Version Info
Last reviewed on: 9/20/2022
Reviewed by: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
