Cluster headache
Histamine headache; Headache - histamine; Migrainous neuralgia; Headache - cluster; Horton's headache; Vascular headache - cluster; Episodic cluster headache; Chronic cluster headache
A cluster headache is an uncommon type of headache. It is one-sided head pain that may involve tearing of the eyes, a droopy eyelid, and a stuffy nose. Attacks last from 15 minutes to 3 hours, occur daily or almost daily for weeks or months. The attacks are separated by pain-free periods that last at least 1 month or longer.
Cluster headaches may be confused with other common types of headaches such as migraines, sinus headache, and tension headache.
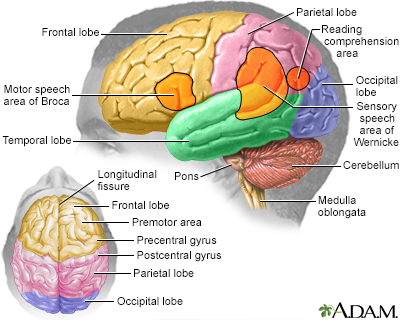
The major areas of the brain have one or more specific functions.
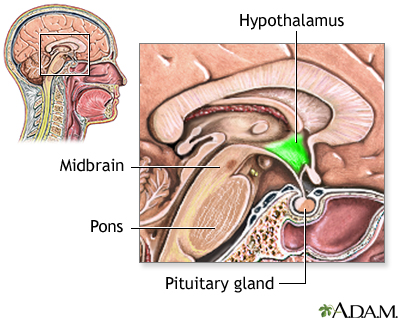
The hypothalamus is a highly complex structure in the brain that regulates many important brain chemicals. Malfunction of this area of the brain may give rise to cluster headaches.
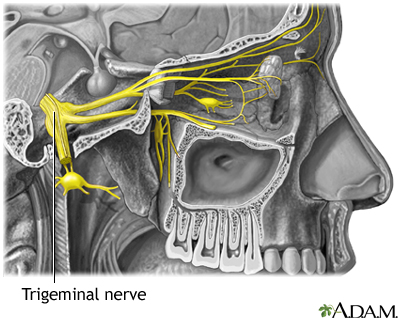
Cluster headaches may be caused by blood vessel dilation in the eye area. Inflammation of nearby nerves may give rise to the distinctive stabbing, throbbing pain usually felt in one eye. The trigeminal nerves branch off the brainstem behind the eyes and send impulses throughout the cranium and face.
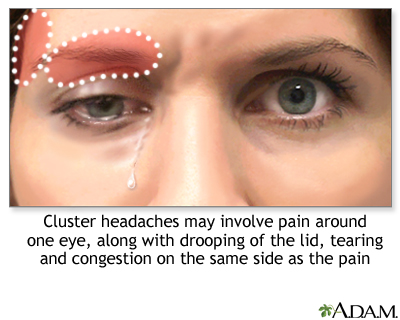
The symptoms of a cluster headache include stabbing severe pain behind or above one eye or in the temple. Tearing of the eye, congestion in the associated nostril, and pupil changes and eyelid drooping may also occur.
Do you sometimes feel really bad pain on one side of your head and face? Do your eyes tear up at the same time? If so, you may be experiencing a cluster headache. Cluster headaches are a fairly common form of repeated headaches. Men get them more often than women, usually in adolescence and middle age. And they tend to run in families. Although we don't know why they happen, they appear to be related to your body releasing chemicals when you encounter things like alcohol, high altitudes, bright light, and heat, among other triggers like certain foods. A cluster headache starts suddenly, and it can be severe. It commonly strikes two to three hours after you fall asleep. But you might get one while you're awake too. Either way, you'll tend to get a headache at the same time of day. The pain typically occurs on one side of your head. You may feel like your head is burning, and the pain will probably be sharp and steady, the worst of it often lasting as long as two hours. You may get headaches daily for months, which is why they're called cluster headaches. Then they may go away for months, only to come back. Your doctor will give you a physical exam and ask questions about your symptoms and medical history. You may need an MRI to rule out other headache causes. Unfortunately, treatment won't cure your cluster headaches, but it should relieve your symptoms. Your doctor will ask you to avoid things that seem to trigger your headaches. You may need medicines such as triptans, several weeks of an anti-inflammatory steroid, oxygen therapy, or even injections of a drug that can stop a headache in five minutes. Call for an appointment with your doctor if cluster headaches do not respond to treatment, if they disturb sleep, if they happen whenever you are active, or are accompanied by other symptoms. Emergency symptoms include drowsiness, vision changes, changes in movement or sensation, seizures, changes in alertness, and nausea or vomiting. Cluster headaches aren't life-threatening, but they ARE chronic and often painful enough to interfere with your work and daily life. But if you don't smoke or drink alcohol, and stay away from other triggers, you can avoid a lot of your headaches.
Causes
Doctors do not know exactly what causes cluster headaches. They seem to be related to the body's sudden release of histamine (chemical in the body released during an allergic response) or serotonin (chemical made by nerve cells) in the area of a nerve in the face called the trigeminal nerve. A problem in a small area at the base of the brain called the hypothalamus may be involved.
More men than women are affected. The headaches can occur at any age, but are most common in the 20s through middle age. They tend to run in families.
Cluster headaches may be triggered by:
- Alcohol and cigarette smoking
- High altitudes (trekking and air travel)
- Bright light (including sunlight)
- Exertion (physical activity)
- Heat (hot weather or hot baths)
- Foods high in nitrites (bacon and preserved meats)
- Certain medicines
- Cocaine
Symptoms
A cluster headache begins as a severe, sudden headache. The headache commonly strikes 2 to 3 hours after you fall asleep. But it can also occur when you are awake. The headache tends to happen daily at the same time of day. Attacks can last for months. They can alternate with periods without headaches (episodic) or they can go on for a year or more without stopping (chronic).
Cluster headache pain is usually:
- Burning, sharp, stabbing, or steady
- Felt on one side of the face from neck to temple, often involving the eye
- At its worst within 5 to 10 minutes, with the strongest pain lasting 30 minutes to 2 hours
When the eye and nose on the same side as the head pain are affected, symptoms can include:
- Swelling under or around the eye (may affect both eyes)
- Excessive tearing
- Red eye
- Droopy eyelid
- Runny nose or stuffy nose on the same side as the head pain
- Red, flushed face, with extreme sweating
Exams and Tests
Your health care provider can diagnose this type of headache by performing a physical exam and asking about your symptoms and medical history.
If a physical exam is done during an attack, the exam will usually reveal Horner syndrome (one-sided eyelid drooping or a small pupil). These symptoms will not be present at other times. No other nervous system (neurologic) changes will be seen.
Tests, such as an MRI of the head, may be needed to rule out other causes of the headaches.
Treatment
Treatment for cluster headaches involves:
- Medicines to treat the pain when it happens
- Medicines to prevent the headaches
TREATING CLUSTER HEADACHES WHEN THEY OCCUR
Your provider may recommend the following treatments for when the headaches occur:
- Triptan medicines, such as sumatriptan (Imitrex).
- Anti-inflammatory (steroid) medicines such as prednisone. Starting with a high dose, then slowly decreasing it over 2 to 3 weeks.
- Breathing in 100% (pure) oxygen.
- Injections of dihydroergotamine (DHE), which can stop cluster attacks within 5 minutes (Warning: this drug can be dangerous if taken with sumatriptan or some other medicines).
You may need more than one of these treatments to control your headache. Your provider may have you try several medicines before deciding which works best for you.
Pain medicines and narcotics do not usually relieve cluster headache pain because they take too long to work.
Surgical treatment may be recommended for you when all other treatments have failed. One such treatment is a neurostimulator. This device delivers tiny electrical signals to certain nerves such as the occipital nerve in the scalp. Your provider can tell you more about surgery.
PREVENTING CLUSTER HEADACHES
Avoid smoking, alcohol use, certain foods, and other things that trigger your headaches. A headache diary can help you identify your headache triggers. When you get a headache, write down the following:
- Day and time the pain began
- What you ate and drank over the past 24 hours
- How much you slept
- What you were doing and where you were right before the pain started
- How long the headache lasted and what made it stop
Review your diary with your provider to identify triggers or a pattern to your headaches. This can help you and your provider create a treatment plan. Knowing your triggers can help you avoid them.
The headaches may go away on their own or you may need treatment to prevent them. The following medicines may also be used to treat or prevent headache symptoms:
- Allergy medicines
- Antidepressants
- Blood pressure medicines
- Seizure medicine
Outlook (Prognosis)
Cluster headaches are not life threatening. They usually do not cause permanent changes to the brain. But they are long-term (chronic), and often painful enough to interfere with work and life. However, they can occur less frequently with age.
When to Contact a Medical Professional
Call 911 if:
- You are experiencing "the worst headache of your life."
- You have speech, vision, or movement problems or loss of balance, especially if you have not had these symptoms with a headache before.
- A headache starts suddenly.
Schedule an appointment or contact your provider if:
- Your headache pattern or pain changes.
- Treatments that once worked no longer help.
- You have side effects from your medicine.
- You are pregnant or could become pregnant. Some medicines should not be taken during pregnancy.
- You need to take pain medicines more than 3 days a week.
- Your headaches are more severe when lying down.
- You have a fever or stiff neck with your headache.
Prevention
If you smoke, now is a good time to stop. Alcohol use and any foods that trigger a cluster headache may need to be avoided. Medicines may prevent cluster headaches in some cases.
References
Garza I, Robertson CE, Smith JH, Whealy MA. Headache and other craniofacial pain. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 102.
Hoffmann J, May A. Diagnosis, pathophysiology, and management of cluster headache. Lancet Neurol. 2018;17(1):75-83. PMID: 29174963
Rozental JM. Tension-type headache, chronic tension-type headache, and other chronic headache types. In: Benzon HT, Raja SN, Liu SS, Fishman SM, Cohen SP, eds. Essentials of Pain Medicine. 4th ed. Philadelphia, PA: Elsevier; 2018:chap 20.
Version Info
Last reviewed on: 11/9/2021
Reviewed by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
