Chronic obstructive pulmonary disease
COPD; Chronic obstructive airways disease; Chronic obstructive lung disease; Chronic bronchitis; Emphysema; Bronchitis - chronic
Chronic obstructive pulmonary disease (COPD) is a common lung disease. Having COPD makes it hard to breathe.
There are two main forms of COPD:
- Chronic bronchitis, which involves a long-term cough with mucus
- Emphysema, which involves damage to the lungs over time
Most people with COPD have a combination of both conditions.

For years, you've enjoyed relaxing with a cigarette in your hand, and looked forward to your cigarette breaks at work, but now, all of that smoking has caught up with you. You're coughing, wheezing, often out of breath. Could you have chronic obstructive pulmonary disease? Let's talk about chronic obstructive pulmonary disease, or COPD, for short. COPD is a lung disease that's usually caused by smoking, although some people who smoke for years never get the condition, while a few get COPD even if they've never lit up. Most people with COPD have a combination of a cough that just won't go away, called chronic bronchitis, and lung damage, called emphysema. The symptoms of COPD can sneak up on you slowly. Over time, you'll develop a cough that lingers, day after day. You'll feel tired, and have trouble catching your breath. Only your doctor can tell for sure whether this is COPD. To test for it, you'll need to breathe or blow into a machine as hard as you can, and hold that breath, as long as you can, in a test called spirometry. You may also need to have a blood test to determine how much oxygen and carbon dioxide is in your blood. If you have COPD, the ways things stand now, you'll have it for life, as there is no cure for this disease. However, there are ways to control the condition and help you breathe more easily. The first thing you do, absolutely need to do, is stop smoking, which will help slow down the damage to your lungs. A few medicines can help relieve COPD symptoms. You may breathe in a bronchodilator medicine through an inhaler to open up your airways, or take steroids to bring down the swelling in your lungs. If you're having real trouble breathing though, call your local emergency services number. You may need to visit the hospital for oxygen or breathing assistance. You may also need to take antibiotics during flare-ups, because getting an infection can make your COPD worse. Though it may be hard to exercise when you're feeling out of breath, staying active will help keep your muscles strong. Your doctor can teach you how to breathe in a different way so that you can exercise with COPD. You can help avoid the shortness of breath, the coughing, and the wheezing of COPD by butting out, kicking your cigarette habit as soon as possible. Not smoking is the absolute best way to prevent COPD. Ask your doctor about programs and medicines that may make it easier for you to quit.

Spirometry is a painless study of air volume and flow rate within the lungs. Spirometry is frequently used to evaluate lung function in people with obstructive or restrictive lung diseases such as asthma or cystic fibrosis.
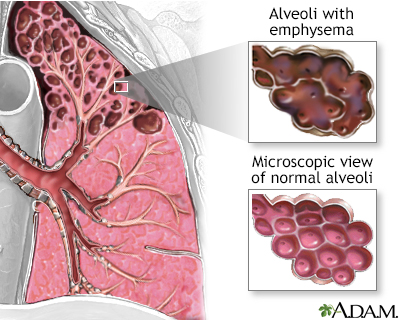
Emphysema is a lung disease involving damage to the air sacs (alveoli). There is progressive destruction of alveoli and the surrounding tissue that supports the alveoli. With more advanced disease, large air cysts develop where normal lung tissue used to be. Air is trapped in the lungs due to lack of supportive tissue which decreases oxygenation.

You probably know by now that smoking damages your lungs, raising your risk for bronchitis, emphysema, and lung cancer. And, you're probably well aware that lighting up also puts you at risk for many different types of cancers, as well as eye disease like cataracts and premature wrinkles, you know why you shouldn't smoke, it's just the quitting part you can't seem to get past. Let's talk about some helpful tips to help you quit smoking, for good this time. It's a familiar story, one that plays out over and over again among smokers. You vow to quit, and you have every intention of doing it, and then the cravings hit. And you can't think about anything but having a cigarette. You get irritable, and you start putting on weight. You think, Just one cigarette wouldn't hurt, would it? And then, before you know it, you're smoking again. Most smokers have tried to quit, and failed, several times. Even if you've failed before, you can still succeed at quitting. Many people have. You just need to find the technique that works for you. So, here are a few tips that can help. First, set a quit date. Write it down on your calendar and tell a few friends, so you'll be too embarrassed to back out. Before your quit date, throw out every cigarette in your house, car, and office. Also toss every ashtray, lighter, and anything else you need to smoke. Wash your clothes and clean your furniture so you won't have that smoky smell hanging around your house. Next, call your doctor. Ask about smoking cessation programs in your area. Also learn about tools that can help you quit, like medicines that reduce the urge to smoke, and nicotine replacement gums, lozenges, patches, and sprays. And then, plan what you'll do instead of smoking. If you smoke with your morning cup of coffee, drink tea or go for a walk instead. If you need a cigarette to keep your mouth busy, try chewing sugarless gum or nibble on a carrot stick. Stick to places where smoking isn't allowed, like smoke-free restaurants. And finally, reward yourself for not smoking. Put all that money that you would have spent on cigarettes into a jar. And once you've collected enough money, use it to take a trip or buy something you've wanted for a long time. Don't get discouraged. Quitting smoking isn't easy. If it were, everyone would have done it by now. Be persistent, reward yourself for the progress you've made, and keep at it until you finally conquer the urge to smoke.
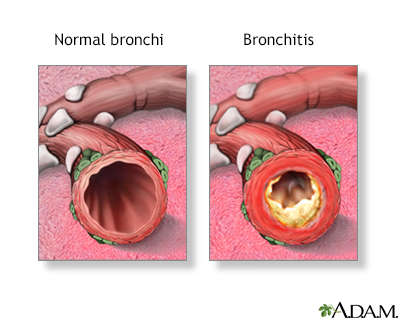
Bronchitis is the inflammation of the bronchi, the main air passages to the lungs. It often results from a respiratory infection caused by a virus or bacteria. Symptoms include coughing, shortness of breath, wheezing and fatigue.
The many methods of quitting smoking include counseling and support groups, nicotine replacement therapy, prescription medications, and incremental reduction.
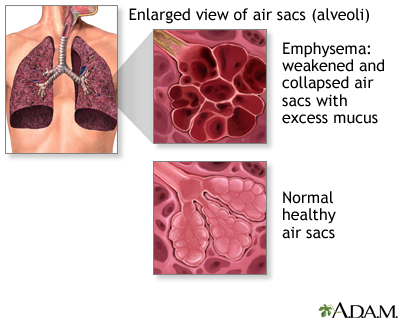
Chronic obstructive pulmonary disease (COPD) refers to chronic lung disorders that result in blocked air flow in the lungs. The two main COPD disorders are emphysema and chronic bronchitis, the most common causes of respiratory failure. Emphysema occurs when the walls between the lung's air sacs become weakened and collapse. Damage from COPD is usually permanent and irreversible.
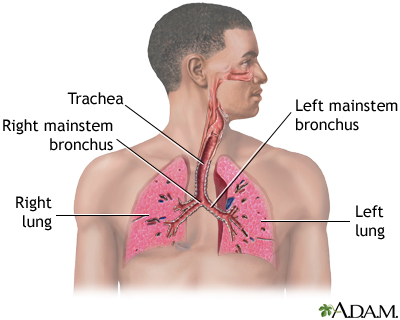
Air is breathed in through the nasal passageways, travels through the trachea and bronchi to the lungs.
For years, you've enjoyed relaxing with a cigarette in your hand, and looked forward to your cigarette breaks at work, but now, all of that smoking has caught up with you. You're coughing, wheezing, often out of breath. Could you have chronic obstructive pulmonary disease? Let's talk about chronic obstructive pulmonary disease, or COPD, for short. COPD is a lung disease that's usually caused by smoking, although some people who smoke for years never get the condition, while a few get COPD even if they've never lit up. Most people with COPD have a combination of a cough that just won't go away, called chronic bronchitis, and lung damage, called emphysema. The symptoms of COPD can sneak up on you slowly. Over time, you'll develop a cough that lingers, day after day. You'll feel tired, and have trouble catching your breath. Only your doctor can tell for sure whether this is COPD. To test for it, you'll need to breathe or blow into a machine as hard as you can, and hold that breath, as long as you can, in a test called spirometry. You may also need to have a blood test to determine how much oxygen and carbon dioxide is in your blood. If you have COPD, the ways things stand now, you'll have it for life, as there is no cure for this disease. However, there are ways to control the condition and help you breathe more easily. The first thing you do, absolutely need to do, is stop smoking, which will help slow down the damage to your lungs. A few medicines can help relieve COPD symptoms. You may breathe in a bronchodilator medicine through an inhaler to open up your airways, or take steroids to bring down the swelling in your lungs. If you're having real trouble breathing though, call your local emergency services number. You may need to visit the hospital for oxygen or breathing assistance. You may also need to take antibiotics during flare-ups, because getting an infection can make your COPD worse. Though it may be hard to exercise when you're feeling out of breath, staying active will help keep your muscles strong. Your doctor can teach you how to breathe in a different way so that you can exercise with COPD. You can help avoid the shortness of breath, the coughing, and the wheezing of COPD by butting out, kicking your cigarette habit as soon as possible. Not smoking is the absolute best way to prevent COPD. Ask your doctor about programs and medicines that may make it easier for you to quit.
Causes
Smoking is the main cause of COPD. The more a person smokes, the more likely that person will develop COPD. But some people smoke for years and never get COPD.
If a person has a rare condition in which they lack a protein called alpha-1 antitrypsin, they can develop emphysema even without smoking.
Other risk factors for COPD are:
- Exposure to certain gases or fumes in the workplace
- Exposure to heavy amounts of secondhand smoke and pollution
- Frequent use of a cooking fire without proper ventilation
Symptoms
Exams and Tests
The best test for COPD is a lung function test called spirometry. This involves blowing out as hard as possible into a small machine that tests air movement and lung capacity. The results can be checked right away.
Using a stethoscope to listen to the lungs can also be helpful, showing prolonged expiratory time or wheezing. But sometimes, the lungs sound normal, even when a person has COPD.
Imaging tests of the lungs, such as x-rays and CT scans may be ordered. With an x-ray, the lungs may look normal, even when a person has COPD. A CT scan will almost always show signs of COPD if it is present.
Sometimes, a blood test called arterial blood gas may be done to measure the amounts of oxygen and carbon dioxide in the blood.
If your health care provider suspects you have alpha-1 antitrypsin deficiency, a blood test will likely be ordered to detect this condition.
Treatment
There is no cure for COPD. But there are many things you can do to relieve symptoms and keep the disease from getting worse.
If you smoke, now is the time to quit. This is the best way to slow lung damage.
Medicines used to treat COPD include:
- Quick-relief drugs to help open the airways
- Control drugs to reduce lung inflammation
- Anti-inflammatory drugs to reduce swelling in the airways
- Certain long-term antibiotics
In severe cases or during flare-ups, you may need to receive:
- Steroids by mouth or through a vein (intravenously)
- Bronchodilators through a nebulizer
- Oxygen therapy
- Assistance from a machine to help breathing by using a mask or through the use of an endotracheal tube
Your provider may prescribe antibiotics during symptom flare-ups, because an infection can make COPD worse.
You may need oxygen therapy at home if you have a low level of oxygen in your blood.
Pulmonary rehabilitation does not cure COPD. But it can teach you more about the disease, train you to breathe in a different way so you can stay active and feel better, and keep you functioning at the highest level possible.
LIVING WITH COPD
You can do things every day to keep COPD from getting worse, protect your lungs, and stay healthy.
Walk to build up strength:
- Ask the provider or respiratory therapist how far to walk.
- Slowly increase how far you walk.
- Avoid talking if you get short of breath when you walk.
- Use pursed lip breathing when you breathe out, to empty your lungs before the next breath.
Things you can do to make it easier for yourself around the home include:
- Avoid very cold air or very hot weather
- Make sure no one smokes in your home
- Reduce air pollution by not using the fireplace and getting rid of other irritants
- Manage stress and your mood
- Use oxygen if prescribed for you
Eat healthy foods, including fish, poultry, and lean meat, as well as fruits and vegetables. If it is hard to keep your weight up, talk to a provider or dietitian about eating foods with more calories, by eating small frequent meals.
Surgery or other interventions may be used to treat COPD. Only a few people benefit from these surgical treatments:
- One-way valves can be inserted with a bronchoscopy to help deflate parts of the lung that are hyperinflated (overinflated) in select patients.
- Surgery to remove parts of the diseased lung, which can help less-diseased parts work better in some people with emphysema (lung volume reduction surgery).
- Lung transplant for a small number of very severe cases.
You probably know by now that smoking damages your lungs, raising your risk for bronchitis, emphysema, and lung cancer. And, you're probably well aware that lighting up also puts you at risk for many different types of cancers, as well as eye disease like cataracts and premature wrinkles, you know why you shouldn't smoke, it's just the quitting part you can't seem to get past. Let's talk about some helpful tips to help you quit smoking, for good this time. It's a familiar story, one that plays out over and over again among smokers. You vow to quit, and you have every intention of doing it, and then the cravings hit. And you can't think about anything but having a cigarette. You get irritable, and you start putting on weight. You think, Just one cigarette wouldn't hurt, would it? And then, before you know it, you're smoking again. Most smokers have tried to quit, and failed, several times. Even if you've failed before, you can still succeed at quitting. Many people have. You just need to find the technique that works for you. So, here are a few tips that can help. First, set a quit date. Write it down on your calendar and tell a few friends, so you'll be too embarrassed to back out. Before your quit date, throw out every cigarette in your house, car, and office. Also toss every ashtray, lighter, and anything else you need to smoke. Wash your clothes and clean your furniture so you won't have that smoky smell hanging around your house. Next, call your doctor. Ask about smoking cessation programs in your area. Also learn about tools that can help you quit, like medicines that reduce the urge to smoke, and nicotine replacement gums, lozenges, patches, and sprays. And then, plan what you'll do instead of smoking. If you smoke with your morning cup of coffee, drink tea or go for a walk instead. If you need a cigarette to keep your mouth busy, try chewing sugarless gum or nibble on a carrot stick. Stick to places where smoking isn't allowed, like smoke-free restaurants. And finally, reward yourself for not smoking. Put all that money that you would have spent on cigarettes into a jar. And once you've collected enough money, use it to take a trip or buy something you've wanted for a long time. Don't get discouraged. Quitting smoking isn't easy. If it were, everyone would have done it by now. Be persistent, reward yourself for the progress you've made, and keep at it until you finally conquer the urge to smoke.
Support Groups
You can ease the stress of illness by joining a support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
COPD is a long-term (chronic) illness. The disease will get worse more quickly if you do not stop smoking.
If you have severe COPD, you will be short of breath with most activities. You may be admitted to the hospital more often.
Talk with your provider about breathing machines and end-of-life care as the disease progresses.
Possible Complications
With COPD, you may have other health problems such as:
- Irregular heartbeat (arrhythmia)
- Need for breathing machine support with a mask (non-invasive ventilation) and oxygen therapy
- Right-sided heart failure or cor pulmonale (heart swelling and heart failure due to chronic lung disease)
- Pneumonia
- Collapsed lung (pneumothorax)
- Severe weight loss and malnutrition
- Thinning of the bones (osteoporosis)
- Debilitation
- Increased anxiety
When to Contact a Medical Professional
Go to the emergency room or call 911 or the local emergency number if you have a rapid increase in shortness of breath.
Prevention
Not smoking prevents most cases of COPD. Ask your provider about quit-smoking programs. Medicines are also available to help you stop smoking.
References
Global Initiative for Chronic Obstructive Lung Disease (GOLD) website. Global Initiative for Chronic Obstructive Lung Disease: 2023 Report.
Han MK, Lazarus SC. COPD: diagnosis and management. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 64.
National Institutes of Health, National Heart, Lung, and Blood Institute website. COPD national action plan.
Rochester CL, Nici L. Pulmonary rehabilitation. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 139.
Version Info
Last reviewed on: 5/3/2023
Reviewed by: Denis Hadjiliadis, MD, MHS, Paul F. Harron, Jr. Professor of Medicine, Pulmonary, Allergy, and Critical Care, Perelman School of Medicine, University of Pennsylvania, Philadelphia, PA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
