Small Wireless Pacemaker is Safe, Effective in Early Testing
Mount Sinai reports promising European study results for new leadless pacemaker it is currently testing in U.S. clinical trial.
A new small, wireless self-contained pacemaker appears safe and feasible for use in patients, according to a new study published by researchers from Icahn School of Medicine at Mount Sinai on March 24 in the American Heart Association journal Circulation.
Although traditional pacemakers pose minimal risk, patients are still vulnerable to some short- or long-term complications, according to Vivek Y. Reddy, MD, lead author of the study and Director of Arrhythmia Services at The Mount Sinai Hospital.
Those complications can stem from the pulse generator implanted under the skin of the chest, where infections or skin breakdown can occur, and particularly from the leads, or wires, that run from the generator through a vein to the heart. Leads can break, dislodge or contribute to a vein blockage.
However, the new pacemaker has no leads — its pulse generator lies within the unit in the heart – and is placed without the need for surgery.
At 6 millimeters in diameter and about 42 millimeters long, the wireless device is smaller than a triple-A battery. It's faster and easier to implant than traditional pacemakers, Dr. Reddy says, and it's programmed and monitored similarly.
"While a much larger study is required to prove this, one may expect the leadless pacemaker to be associated with less chance of infection and lead-related problems such as lead fracture," says Dr. Reddy. "Overall, the self-contained pacemaker is a paradigm shift in cardiac pacing."
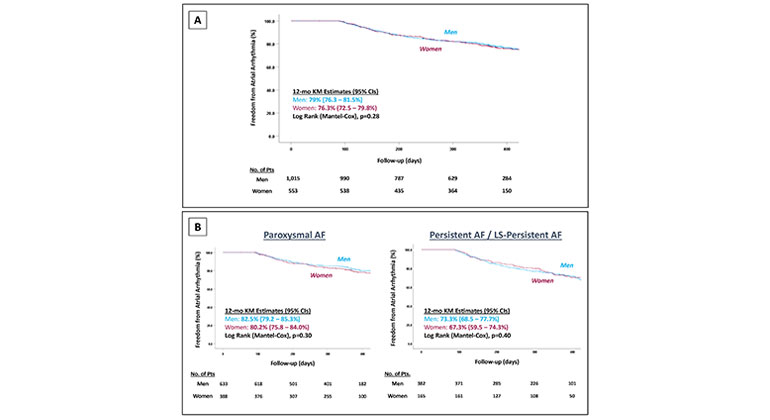
The study, called LEADLESS, was conducted in 33 Caucasian patients, average age 77, two-thirds men, at two hospitals in Prague and one in Amsterdam. The self-contained pacemaker was successfully implanted in 32 patients, or 97 percent. Ninety-four percent were free of complications through the three-month study period, the researchers reported.
The new device is a self-modulating pacer guided into place using a catheter inserted in the femoral vein and is affixed to the heart in the right ventricle, the same place a standard lead would be located. The device is for patients who require single-chamber pacing, or roughly 20 percent to 30 percent of United States and European patients who need pacemakers. Patients who need dual-chamber pacing would still require traditional pacemakers, according to Dr. Reddy.
Among the study's 33 patients, one suffered complications during the procedure and underwent emergency surgery but later died after suffering a stroke.
After three months, the new pacemakers were functioning well, the researchers found. They are continuing to track the patients and expect to report longer-term outcomes later this year. Meanwhile, a much larger study at multiple U.S. locations that will include longer-term follow-up is under way, says Dr. Reddy.
In February, Dr. Reddy launched the LEADLESS II clinical research trial after implanting the United States' first leadless pacemaker at The Mount Sinai Hospital. LEADLESS II is planning to enroll 670 patients at 50 centers across the U.S., Canada, and Europe.
The co-authors of the newly published LEADLESS study findings include: Reinoud E. Knops, MD; Johannes Sperzel, MD; Marc A. Miller, MD; Jan Petru, MD; Jaroslav Simon, MD; Lucie Sediva, MD; Joris R. de Groot, MD, PhD; Fleur V.Y. Tjong, MD; Peter Jacobson, BS; Alan Ostrosff, MS; Srinivas R. Dukkipati, MS; Jacob S. Koruth, MD; Arthur A.M. Wilde, MD, PhD; Josef Kautzner, MD, PhD; and Petr Neuzil, MD, PhD.
The study was funded by St. Jude Medical, the manufacturer of the Nanostim pacemaker.
Dr. Reddy receives financial compensation as a consultant and advisory board member for St. Jude Medical, the study sponsor and manufacturer of the Nanostim pacemaker system being evaluated in this study. In addition, in 2013 he received one-time financial compensation from St. Jude Medical in the form of an option buyout relating to St. Jude Medical's acquisition of Nanostim.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.

Inter-Atrial Shunts May Benefit Some Heart Failure Patients While Harming Others
Apr 06, 2024 View All Press Releases
Ismail El-Hamamsy, MD, PhD, Named President of the Heart Valve Society
Feb 22, 2024 View All Press Releases