First Leadless Pacemaker in United States Implanted into a Patient at The Mount Sinai Hospital
Vivek Reddy, MD, launches international LEADLESS II clinical research trial testing a miniature-sized, leadless pacemaker placed inside the heart without surgery.
This February during American Heart Month, Vivek Reddy, MD, of Mount Sinai Heart at The Mount Sinai Hospital implanted the United States' first miniature-sized, leadless cardiac pacemaker directly inside a patient's heart without surgery.
The leads-free pacemaker is implanted by a cardiac electrophysiologist directly inside the heart during a catheter-guided procedure through the groin via the femoral vein. The device, resembling a small, metal silver tube, is only a few centimeters in length, making it less than ten percent the size of a traditional pacemaker.
The Nanostim device, made by St. Jude Medical, is being tested for safety and efficacy in an international, multicenter clinical trial called LEADLESS II, which is planning to enroll 670 patients at 50 centers across the U.S., Canada, and Europe.
"This clinical research trial will be testing the latest innovative, non-surgical pacemaker option for patients experiencing a slowed heart beat," says Vivek Reddy, MD, the study's co-investigator who is Director of Electrophysiology Services at The Mount Sinai Hospital and Chairman of the Steering Committee of the study. "This new-age, tiny pacemaker may ultimately be safer for patients because it doesn't have leads or have to be inserted under the skin of a patient's chest, like a traditional cardiac pacemaker."
Similar to other cardiac pacemakers, the Nanostim device treats a heart rate that is too slow called bradycardia. It works by closely monitoring the heart's electrical rhythms and if the heart beat is too slow it provides electrical stimulation therapy to regulate it. More than 4 million patients globally have a pacemaker, and 700,000 new patients receive one each year.
The possible advantages of the leadless pacemaker include the elimination of a surgical pocket and no visible pacemaker device under a patient's chest skin, no incision scar on the chest, no connector wires or leads, and no restrictions on a patient's activities. The device's benefits may also allow for less patient discomfort, infections, and device complications and dysfunction. In addition, the free-standing, battery-operated pacemaker device is designed to be fully retrievable from the heart.
"The same cardiac pacing results for patients may be available with this smaller leads-free device with the added benefits of a non-surgical procedure and less complication risks," says Srinivas Dukkipati, MD, Co-Director of Electrophysiology Services at The Mount Sinai Hospital, who is the study's principal investigator at The Mount Sinai Hospital. "The new pacemaker may also improve a patient's quality of life allowing them to live a more active lifestyle since the device is more safely hidden away deep inside their heart."
"I believe this pioneering, compact device, which is placed directly inside the heart, may be a true game-changing technology in cardiovascular medicine that may help revolutionize care for patients with arrhythmias," adds Dr. Reddy. "I look forward to the results of the LEADLESS II clinical trial. Previous initial research testing of the device already showed overall its performance is comparable to traditional pacemakers."
"Since establishing the Helmsley Center for Electrophysiology in 2009, Mount Sinai Heart's Electrophysiology team has been bringing the most advanced healthcare technologies and therapies to our patients," says Valentin Fuster, MD, PhD, Director of Mount Sinai Heart, Physician-in-Chief of The Mount Sinai Hospital, and the next Editor-in-Chief of The Journal of the American College of Cardiology (JACC). "The leadless pacemaker is the latest example of this cutting-edge work being performed by Dr. Reddy, Dr. Dukkipati, and the rest of the Electrophysiology team at Mount Sinai."
Dr. Reddy receives financial compensation as a consultant and advisory board member for St. Jude Medical, the study sponsor and manufacturer of the Nanostim pacemaker system being evaluated in this study. In addition, in 2013 he received one-time financial compensation from St. Jude Medical in the form of an option buyout relating to St. Jude Medical's acquisition of Nanostim.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
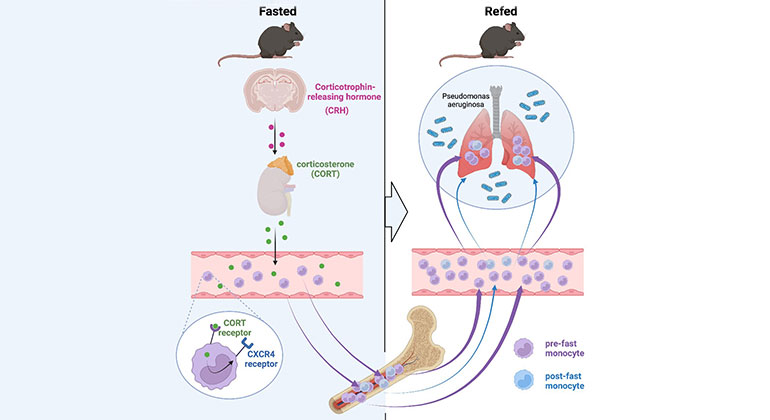
Skipping Breakfast May Compromise the Immune System
Feb 23, 2023 View All Press Releases
Valentin Fuster, MD, PhD, Receives Prestigious Award from City of Barcelona, Spain
Jan 23, 2023 View All Press Releases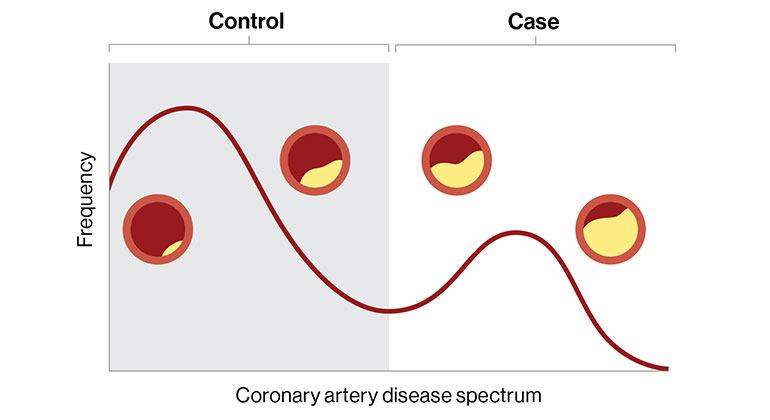
Digital Marker for Coronary Artery Disease Built by Researchers at Mount Sinai
Dec 20, 2022 View All Press Releases
Samin Sharma, MD, Named Director of the Mount Sinai Cardiovascular Clinical Institute
Nov 28, 2022 View All Press Releases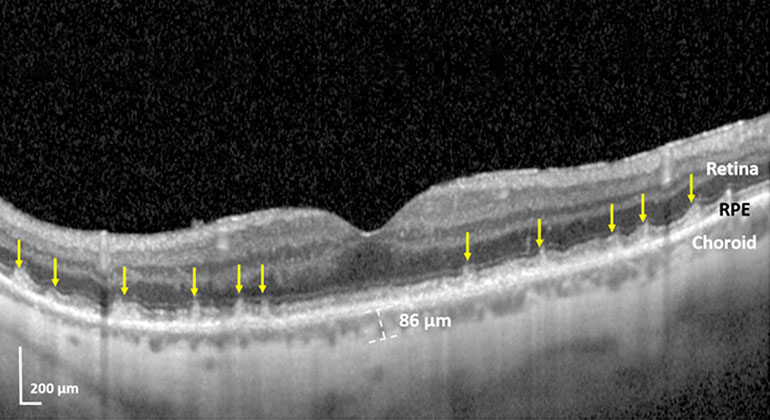
Blinding Eye Disease Strongly Associated With Serious Forms of Cardiovascular Disease
Nov 17, 2022 View All Press Releases




