Delivery of Stem Cells into Heart Muscle After Heart Attack May Enhance Cardiac Repair and Reverse Injury
Mount Sinai's Cardiovascular Research Center presents new findings at the AHA Scientific Sessions 2014.
Delivering stem cell factor directly into damaged heart muscle after a heart attack may help repair and regenerate injured tissue, according to a study led by researchers from Icahn School of Medicine at Mount Sinai presented November 18 at the American Heart Association Scientific Sessions 2014 in Chicago, IL.
"Our discoveries offer insight into the power of stem cells to regenerate damaged muscle after a heart attack,"says lead study author Kenneth Fish, PhD, Director of the Cardiology Laboratory for Translational Research, Cardiovascular Research Center, Mount Sinai Heart, Icahn School of Medicine at Mount Sinai.
In the study, Mount Sinai researchers administered stem cell factor (SCF) by gene transfer shortly after inducing heart attacks in pre-clinical models directly into damaged heart tissue to test its regenerative repair response. A novel SCF gene transfer delivery system induced the recruitment and expansion of adult c-Kit positive (cKit+) cardiac stem cells to injury sites that reversed heart attack damage. In addition, the gene therapy improved cardiac function, decreased heart muscle cell death, increased regeneration of heart tissue blood vessels, and reduced the formation of heart tissue scarring.
"It is clear that the expression of the stem cell factor gene results in the generation of specific signals to neighboring cells in the damaged heart resulting in improved outcomes at the molecular, cellular, and organ level," says Roger J. Hajjar, MD, senior study author and Director of the Cardiovascular Research Center at Mount Sinai. "Thus, while still in the early stages of investigation, there is evidence that recruiting this small group of stem cells to the heart could be the basis of novel therapies for halting the clinical deterioration in patients with advanced heart failure."
cKit+ cells are a critical cardiac cytokine, or protein receptor, that bond to stem cell factors. They naturally increase after myocardial infarction and through cell proliferation are involved in cardiac repair.
According to researchers there has been a need for the development of interventional strategies for cardiomyopathy and preventing its progression to heart failure. Heart disease is the number one cause of death in the United States, with cardiomyopathy or an enlarged heart from heart attack or poor blood supply due to clogged arteries being the most common causes of the condition. In addition, cardiomyopathy causes a loss of cardiomyocyte cells that control heartbeat, and changes in heart shape, which lead to the heart’s decreased pumping efficiency.
"Our study shows our SCF gene transfer strategy can mobilize a promising adult stem cell type to the damaged region of the heart to improve cardiac pumping function and reduce myocardial infarction sizes resulting in improved cardiac performance and potentially increase long-term survival and improve quality of life in patients at risk of progressing to heart failure," says Dr. Fish.
"This study adds to the emerging evidence that a small population of adult stem cells can be recruited to the damaged areas of the heart and improve clinical outcomes," says Dr. Hajjar.
Other study co-authors included Kiyotake Ishikawa, MD, Jaume Aguero, MD, Lisa Tilemann, MD, Dongtak Jeong, PhD, Lifan Liang, PhD, Lauren Fish, Elisa Yaniz-Galende, PhD, and Krisztina Zsebo, PhD.
This research study was performed in collaboration with the Celladon Corporation in San Diego, CA. Dr. Hajjar is the scientific cofounder of the company Celladon, which is developing his AAV1/SERCA2a gene therapy for the treatment of heart failure. He holds equity in Celladon and receives financial compensation as a member of its advisory board.
Abstract 17141 was presented at the AHA Scientific Sessions 2014 as: Stem Cell Factor Gene Transfer in a Swine Model of Ischemic Cardiomyopathy is accompanied by decreased apoptosis and proliferating cKit cells.
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
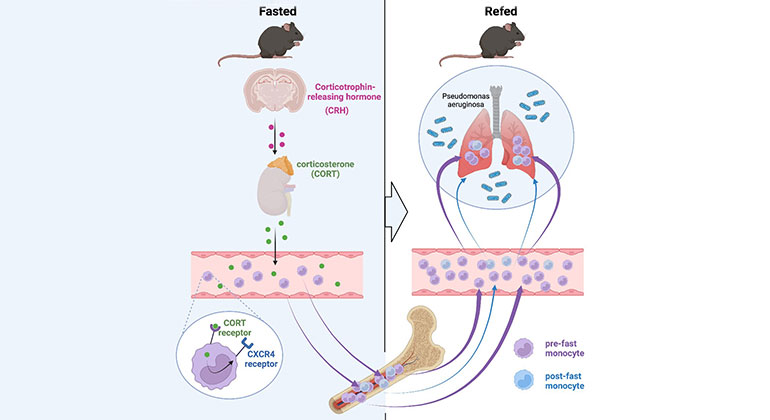
Skipping Breakfast May Compromise the Immune System
Feb 23, 2023 View All Press Releases
Mount Sinai Recruits Internationally Recognized Cardiovascular Immunology Researcher
Jul 21, 2021 View All Press Releases

.jpg)