Researchers Identify First Drug Targets in Childhood Genetic Tumor Disorder
Two mutations central to the development of infantile myofibromatosis may provide new therapeutic targets.
Two mutations central to the development of infantile myofibromatosis (IM)—a disorder characterized by multiple tumors involving the skin, bone, and soft tissue—may provide new therapeutic targets, according to researchers from the Icahn School of Medicine at Mount Sinai. The findings, published in The American Journal of Human Genetics, may lead to new treatment options for this debilitating disease, for which the only current treatment option is repeated surgical removal of the tumors.
IM is an inheritied disorder that develops in infancy or even in utero and tumors continue to present throughout life. The tumors do not metastasize, but can grow large enough to invade the tissue surrounding them causing physical limitations, disfiguration, bone destruction, intestitinal obstruction, and even death. Currently, the standard of care is to excise the tumors when possible, which can be invasive, painful, and disfiguring, and most patients require multiple surgeries throughout their lives.
Led by John Martignetti, MD, PhD, Associate Professor of Genetics and Genomic Sciences, Oncological Sciences, and Pediatrics and other researchers at the Icahn School of Medicine at Mount Sinai and Hakon Hakonarson, MD, PhD at the Children’s Hospital of Philadelphia, the global research team gathered blood samples from 32 people from nine different families affected by the disease and performed whole-exome sequencing, a type of genomic sequencing where all protein coding regions of the genome, called the exome, are analyzed. They identified mutations in two genes: PDGFRB and NOTCH3.
“We are very excited about the findings of this study, which started 10 years ago with the enrollment of the first family,” said Dr. Martignetti. “The newest developments in sequencing technology have led to a new breakthrough in understanding this debilitating disease and we can therefore begin identifying drug-based treatments to save lives for some and avoiding the negative quality of life impact of extensive and repeated surgery in others.”
PDGFRB and NOTCH3 are two genes that are targeted by existing drugs, including imatinib (GLEEVEC®) and sunitinib (Sutent®). Next, Dr. Martignetti and his team plans to test whether cells grown in the laboratory from myfibromatosis tumors are susceptible to these drugs. They also hope to learn why mutations in these two genes result in disease.“If we can learn how these mutated genes get hijacked to cause cellular miscommunication, and also test existing and novel therapies to see if they shrink the tumors, we hope to improve the lives of the individuals battling this disease,” said Dr. Martignetti.
About The Mount Sinai Medical Center
The Mount Sinai Medical Center encompasses both The Mount Sinai Hospital and Icahn School of Medicine at Mount Sinai. Established in 1968, the Icahn School of Medicine at Mount Sinai is one of the leading medical schools in the United States. The Icahn School of Medicine is noted for innovation in education, biomedical research, clinical care delivery, and local and global community service. It has more than 3,400 faculty members in 32 departments and 14 research institutes, and ranks among the top 20 medical schools both in National Institutes of Health (NIH) funding and by U.S. News & World Report.
The Mount Sinai Hospital, founded in 1852, is a 1,171-bed tertiary- and quaternary-care teaching facility and one of the nation’s oldest, largest and most-respected voluntary hospitals. In 2012, U.S. News & World Report ranked The Mount Sinai Hospital 14th on its elite Honor Roll of the nation’s top hospitals based on reputation, safety, and other patient-care factors. Mount Sinai is one of just 12 integrated academic medical centers whose medical school ranks among the top 20 in NIH funding and by U.S. News & World Report and whose hospital is on the U.S. News & World Report Honor Roll. Nearly 60,000 people were treated at Mount Sinai as inpatients last year, and approximately 560,000 outpatient visits took place.
For more information, visit http://www.mountsinai.org.
Find Mount Sinai on:
Facebook: http://www.facebook.com/mountsinainyc
Twitter @mountsinainyc
YouTube: http://www.youtube.com/mountsinainy
# # #
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
New RNA-based Therapy Combats Melanoma in Mouse Models
Jul 27, 2023 View All Press Releases
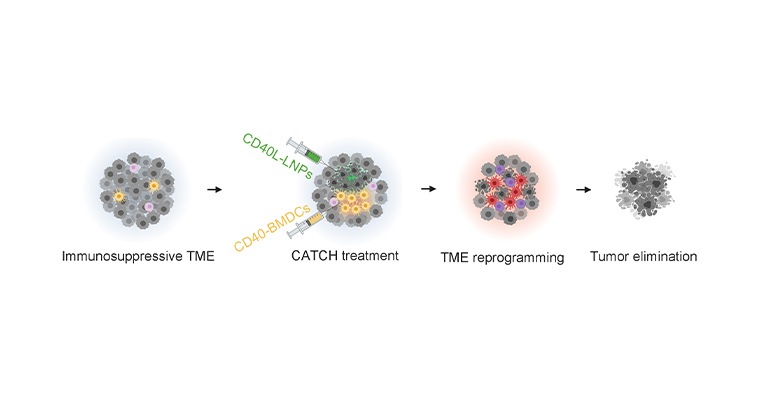
Targeting One Type of Immune Cell With Another Slows Cancer Growth in Preclinical Studies
Oct 25, 2022 View All Press Releases
Novel CRISPR Imaging Technology Reveals Genes Controlling Tumor Immunity
Mar 15, 2022 View All Press ReleasesMount Sinai Researchers: Why COVID-19 May Be Less Common in Children Than Adults
May 22, 2020 View All Press ReleasesAirway Microbiome and Host Interact Differently in Children with Severe Asthma
Mar 12, 2020 View All Press Releases