Protein Lost in Tumors Blocks Normal Cells From Being Reprogrammed into Stem Cells
Mount Sinai researchers identify mechanism that prevents cells from being reprogrammed into embryonic stem cells
Researchers from the Icahn School of Medicine at Mount Sinai have discovered that a particular protein prevents normal cells from being reprogrammed into cells that resemble stem cells, providing new insight into how they may lose their plasticity during normal development. This finding has broad-reaching implications for how cells change during both normal and disease development. The data are published this week in Nature Communications.
In a previous study, Emily Bernstein, PhD, and her team at Mount Sinai studied the natural progression of melanoma using mouse and human cells, as well as patient samples, and found that the loss of a specific histone variant called macroH2A, which is a protein that helps package DNA, was directly related to the growth and metastasis of melanoma. In the current study, her team wanted to find out how this molecule might act as a barrier to cellular reprogramming. The importance of cellular reprogramming has been recently highlighted by the winners of the Nobel Prize of Medicine (2012), and explores the capacity of reversing adult cells to an early stage of development, the so called embryonic stem cell.
Working with researchers at the University of Pennsylvania, Dr. Bernstein evaluated mice that were genetically engineered to lack macroH2A in comparison to control or “wild-type” mice. They used skin cells from these mice and attempted to reprogram the cells in petri dishes into pluripotent cells. They found that the cells derived from mice without macroH2A were much more plastic, meaning they were more easily reprogrammed into stem-like cells, compared to the wild-type mice. This indicates that macroH2A may block cellular reprogramming by silencing genes required for plasticity.
“This is the first evidence of the involvement of a histone variant protein as an epigenetic barrier to induced pluripotency (iPS) reprogramming,” said Dr. Bernstein, who is an Assistant Professor of Oncological Sciences and Dermatology at the Graduate School of Biomedical Sciences at Mount Sinai, and corresponding author of the study. “These findings help us to understand the progression of different cancers and how macroH2A might be acting as a barrier to tumor development.”
Next, Dr. Bernstein and her team plan to create cancer cells in a petri dish by manipulating healthy cells with genetic mutations often associated with cancer, coupled to removal of macroH2A to examine whether the cells are capable of forming tumors.
This study was supported by funding from a New York State Stem Cell Science Award (C024285) and a National Institutes of Health Grant (R01CA154683).
About The Mount Sinai Medical Center
The Mount Sinai Medical Center encompasses both The Mount Sinai Hospital and Icahn School of Medicine at Mount Sinai. Established in 1968, the Icahn School of Medicine is one of the leading medical schools in the United States, and is noted for innovation in education, biomedical research, clinical care delivery, and local and global community service. It has more than 3,400 faculty in 32 departments and 14 research institutes, and ranks among the top 20 medical schools both in National Institutes of Health (NIH) funding and by U.S. News & World Report.
The Mount Sinai Hospital, founded in 1852, is a 1,171-bed tertiary- and quaternary-care teaching facility and one of the nation’s oldest, largest and most-respected voluntary hospitals. In 2012, U.S. News & World Report ranked The Mount Sinai Hospital 14th on its elite Honor Roll of the nation’s top hospitals based on reputation, safety, and other patient-care factors. Mount Sinai is one of 12 integrated academic medical centers whose medical school ranks among the top 20 in NIH funding and by U.S. News & World Report and whose hospital is on the U.S. News & World Report Honor Roll. Nearly 60,000 people were treated at Mount Sinai as inpatients last year, and approximately 560,000 outpatient visits took place.
For more information, visit http://www.mountsinai.org.
Find Mount Sinai on:
Facebook: http://www.facebook.com/mountsinainyc
Twitter @mountsinainyc
YouTube: http://www.youtube.com/mountsinainy
# # #
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
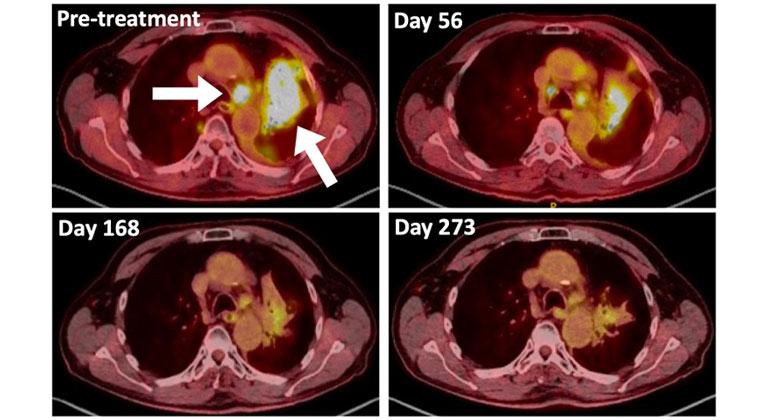
A Type of Allergy Medicine Might Help Treat Lung Cancer, Research Suggests
Dec 06, 2023 View All Press Releases
Diabetes May Accelerate Blood Cancer Growth, Yet Survival Outcomes Differ by Race
Sep 29, 2023 View All Press Releases
Mount Sinai Awarded $3.4 Million to Study Prostate Cancer in People With HIV
Sep 12, 2023 View All Press Releases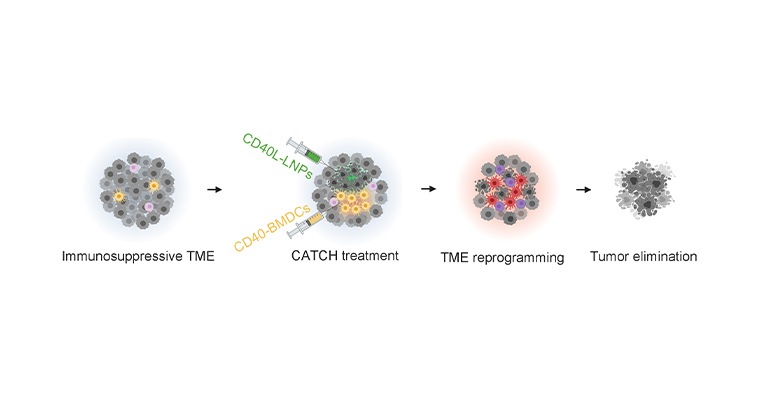
New RNA-based Therapy Combats Melanoma in Mouse Models
Jul 27, 2023 View All Press Releases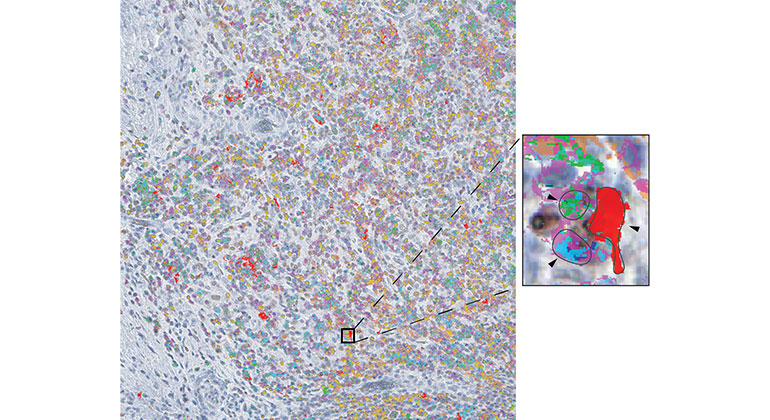
Study Reveals a Trio of Immune Cells Vital in Response to Liver Cancer Immunotherapy
Jun 15, 2023 View All Press Releases


