National Institute of Neurological Disorders and Stroke (NINDS) Stops Enrolling Patients in ARUBA Study Earlier than Planned
Mount Sinai’s International Center for Health Outcomes and Innovation Research (InCHOIR) is the data-coordinating center for the trial
Today the National Institute of Neurological Disorders and Stroke (NINDS) announced that "A Randomized Trial of Unruptured Brain Arteriovenous Malformations" (ARUBA) has stopped enrolling patients because of higher than expected event rates in the interventional therapy arm.
The International Center for Health Outcomes and Innovation Research (InCHOIR) at the Icahn School of Medicine at Mount Sinai is the international data-coordinating center for the trial. "We have discovered that, in an interim analysis of the data collected so far, medical management was superior to interventional therapy for patients with unruptured brain arteriovenous malformations," said Alan J. Moskowitz, MD, Professor and Vice Chair of Health Evidence and Policy at the Icahn School of Medicine, and Co-Director of InCHOIR). "It is our recommendation that extended follow-up is needed to determine whether these disparities in rates will persist over time."
The data, analyzed by InCHOIR under the direction of Michael Parides, PhD, Director of the Center for Biostatistics at the Icahn School of Medicine at Mount Sinai, has shown that after a mean follow-up of 33 months, the event rate in the intervention group was more than three times higher than in the medical management group. The analysis included data from 224 participants enrolled in the study’s 39 worldwide sites, in an effort that was coordinated by Ellen Moquete, RN, BSN, Director of Trials Operations at InCHOIR. Originally the study planned to enroll 400 participants, however, because of the higher than expected event rate in the interventional therapy arm, the ARUBA Data and Safety Monitoring Board has recommended stopping enrollment while continuing to follow those in the study to see if the difference changes over time.
Another key endpoint in the trial is functional status, said Dr. Parides. "Continued follow-up of patients will help determine whether the observed differences in event rates will translate into meaningful long-term differences in patient functioning."
ARUBA is a randomized, multi-center trial designed to evaluate whether symptomatic medical management improves long-term outcomes of patients with unruptured brain arteriovenous malformations compared to invasive treatment for the composite event of death from any cause or symptomatic stroke. There will be a detailed analysis of the data as well as further results presented at the European Stroke Conference in London on May 31.
The Mount Sinai Medical Center
The Mount Sinai Medical Center encompasses both The Mount Sinai Hospital and Icahn School of Medicine at Mount Sinai. Established in 1968, the Icahn School of Medicine is one of the leading medical schools in the United States. The Medical School is noted for innovation in education, biomedical research, clinical care delivery, and local and global community service. It has more than 3,400 faculty in 32 departments and 14 research institutes, and ranks among the top 20 medical schools both in National Institutes of Health (NIH) funding and by U.S. News & World Report.
The Mount Sinai Hospital, founded in 1852, is a 1,171-bed tertiary- and quaternary-care teaching facility and one of the nation’s oldest, largest and most-respected voluntary hospitals. In 2011, U.S. News & World Report ranked The Mount Sinai Hospital 16th on its elite Honor Roll of the nation’s top hospitals based on reputation, safety, and other patient-care factors. Of the top 20 hospitals in the United States, Mount Sinai is one of 12 integrated academic medical centers whose medical school ranks among the top 20 in NIH funding and U.S. News & World Report and whose hospital is on the U.S. News & World Report Honor Roll. Nearly 60,000 people were treated at Mount Sinai as inpatients last year, and approximately 560,000 outpatient visits took place.
For more information, visit http://www.mountsinai.org/
Find Mount Sinai on Facebook, Twitter and YouTube
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
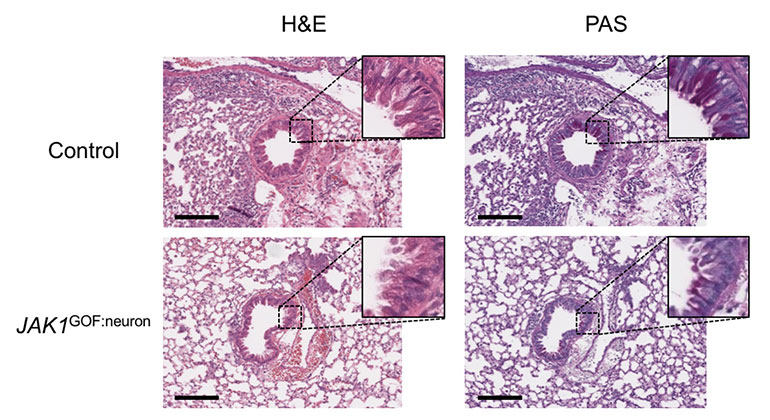
New Insights Revealed On Tissue-Dependent Roles of JAK Signaling in Inflammation
Dec 21, 2023 View All Press Releases