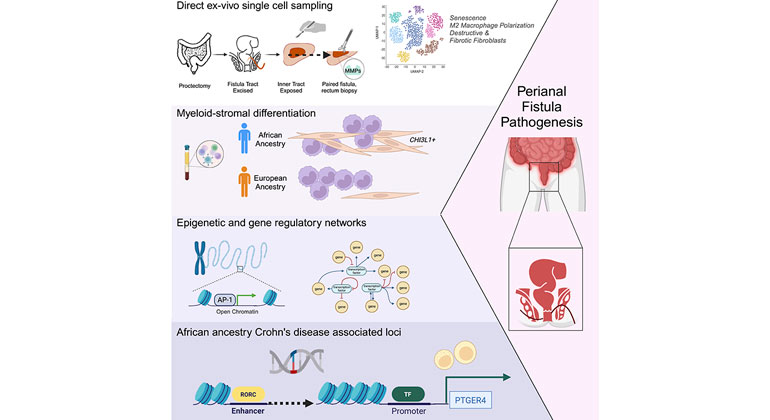
Blocking Sugar Intake May Reduce Cancer Risk or Progression in Obese and Diabetic People
Findings reveal why patients with metabolism-related diseases are at higher risk for aggressive tumors
Blocking dietary sugar and its activity in tumor cells may reduce cancer risk and progression, according to researchers from the Icahn School of Medicine. The study, conducted in fruit flies and published in the journal Cell, provides insight as to why metabolism-related diseases such as diabetes or obesity are associated with certain types of cancer, including pancreatic, breast, liver, and colon cancers.
Ross Cagan, PhD, Professor of Developmental and Regenerative Biology at Mount Sinai, has developed a cancer model in the fruit fly Drosophila that allows scientists to evaluate diseases in the context of the whole animal and multiple genetic targets, rather than just looking at the connection of one gene to one disease. In the current study, Dr. Cagan used fruit flies to understand the effects of diet and insulin resistance on cancer progression.
Cells use glucose for energy and to grow. When a cell becomes insulin resistant, glucose builds up in the blood instead of being absorbed by the cell, starving the cell and leading to metabolic diseases like diabetes. Because of this dysfunctional growth, scientists have been puzzled about how tumors can thrive in an insulin-resistant environment.
“Previous research has established a strong correlation between metabolic diseases and pancreatic, breast, liver, and colon cancers, but we have not determined how tumors grow so aggressively in this environment if they do not have the energy provided by glucose,” said Dr. Cagan, who is also Associate Dean of the Graduate School of Biomedical Sciences at Mount Sinai. “Using our fruit fly model, we discovered how tumors overcome insulin resistance in the body and turn metabolic dysfunction to their advantage.”
Dr. Cagan and his team engineered fruit flies to express Ras and Src, two important oncogenes, resulting in the development of small head tumors. Next, they fed the flies with a high-sugar diet that promoted insulin resistance. They found that high dietary sugar acts together with Ras and Src to increase insulin sensitivity specifically in tumor cells. By ramping up signaling of an important pathway called Wingless/Wnt, they increased tumor cells’ insulin receptors to further promote insulin sensitivity. This cascade of activity changed these small, weak tumors and caused them to begin growing aggressively.
Armed with three new drug targets—glucose, the Ras/Src oncogenes, and Wingless/Wnt signaling—Dr. Cagan and his team identified compounds that can block the process. They treated the flies with acarbose, a treatment for diabetes; a compound called AD81; and a drug called pyrvinium. Acarbose blocked sugar conversion to glucose; AD81 cut off Ras/Src and caused cell death; and pyrvinium inhibited Wingless/Wnt signaling. Taken together, this cocktail of drugs substantially reduced tumor size and progression.
“Our study shows that sugar activates oncogenes in the tumor, which then promote insulin sensitivity, meaning that the exorbitant glucose levels in the blood pour into the tumor, having nowhere else to go in the insulin-resistant body,” said Dr. Cagan. “We have identified a three-drug combination that stops this signaling activity and tumor growth in its tracks, without affecting normal cell function.”
Next, the research team plans to find out whether the same cascade of events is happening in humans with insulin resistance using tumor samples. Based on those findings, Dr. Cagan and his team will test compounds that exploit this oncogene/sugar cascade.
This work was supported through multiple grants from the National Institutes of Health.
###
About the Mount Sinai Health System
Mount Sinai Health System is one of the largest academic medical systems in the New York metro area, with more than 43,000 employees working across eight hospitals, over 400 outpatient practices, nearly 300 labs, a school of nursing, and a leading school of medicine and graduate education. Mount Sinai advances health for all people, everywhere, by taking on the most complex health care challenges of our time — discovering and applying new scientific learning and knowledge; developing safer, more effective treatments; educating the next generation of medical leaders and innovators; and supporting local communities by delivering high-quality care to all who need it.
Through the integration of its hospitals, labs, and schools, Mount Sinai offers comprehensive health care solutions from birth through geriatrics, leveraging innovative approaches such as artificial intelligence and informatics while keeping patients’ medical and emotional needs at the center of all treatment. The Health System includes approximately 7,300 primary and specialty care physicians; 13 joint-venture outpatient surgery centers throughout the five boroughs of New York City, Westchester, Long Island, and Florida; and more than 30 affiliated community health centers. We are consistently ranked by U.S. News & World Report's Best Hospitals, receiving high "Honor Roll" status, and are highly ranked: No. 1 in Geriatrics and top 20 in Cardiology/Heart Surgery, Diabetes/Endocrinology, Gastroenterology/GI Surgery, Neurology/Neurosurgery, Orthopedics, Pulmonology/Lung Surgery, Rehabilitation, and Urology. New York Eye and Ear Infirmary of Mount Sinai is ranked No. 12 in Ophthalmology. U.S. News & World Report’s “Best Children’s Hospitals” ranks Mount Sinai Kravis Children's Hospital among the country’s best in several pediatric specialties.
For more information, visit https://www.mountsinai.org or find Mount Sinai on Facebook, Twitter and YouTube.
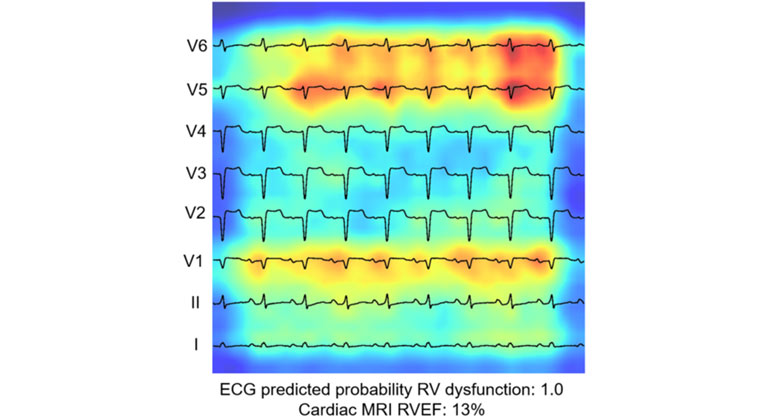
AI-Driven Study Redefines Right Heart Health Assessment With Novel Predictive Model
Jan 04, 2024 View All Press Releases
Demystifying a Key Receptor in Substance Use and Neuropsychiatric Disorders
Jan 02, 2024 View All Press Releases